Making proCHWs the Norm Worldwide
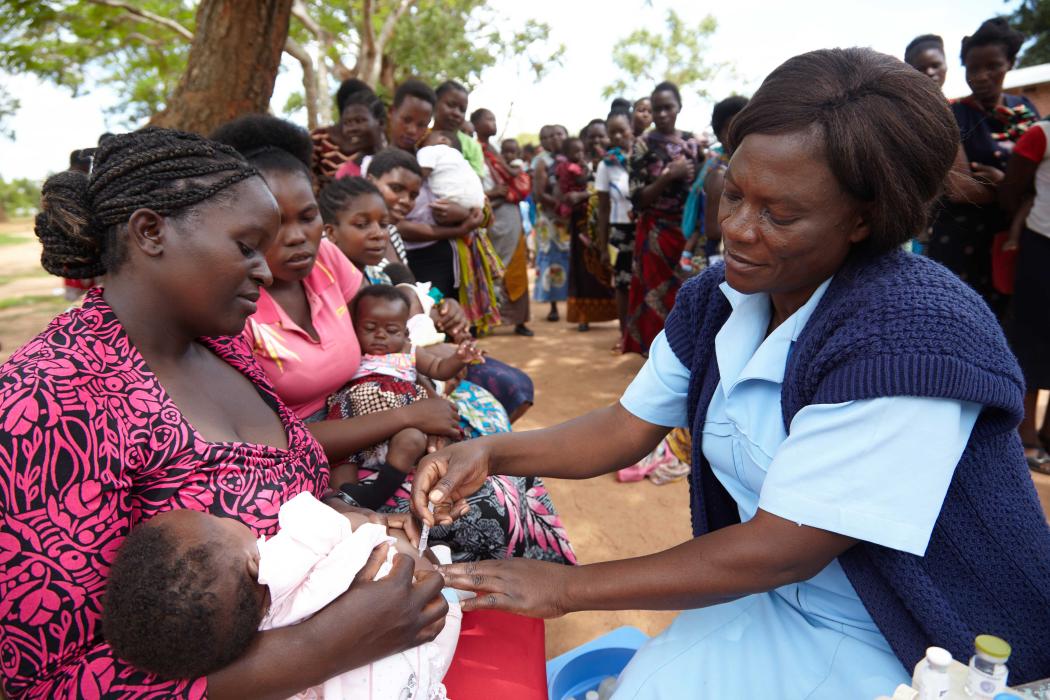
Photo courtesy Community Health Impact Coalition
Despite decades of global health investment, at least half of the people around the world cannot obtain essential health services. They live in both rural and urban areas, commonly defined as the hardest-to-reach communities. The traditional model demands that families find their way to a doctor or hospital for their health care needs. But millions of families live hours—sometimes days—from the nearest clinic.
The standard solution—building more clinics and hiring more doctors—is insufficient. New clinics have conspicuously failed to reach those living in the most remote communities. Health for all requires delivery for every person in every village. And we can get there by seeking new opportunities in an old idea: community health workers (CHWs).
This week, we're recognizing, celebrating, and advocating for targeted actions to support CHWs at the 3rd International Community Health Workforce Symposium in Liberia. At the Symposium, over 500 policymakers, funders, advocates, NGO representatives, and CHWs from across the world are convening to share best practices and catalyze progress on how to provide the policy and systems support—including salaries, skills, supervision, and supplies—that CHWs need to deliver quality care for all.
CHWs are trusted members of the community. Laypeople who have received organized training to provide health care services to neighbors. A link between the health system and individuals. CHWs provide reliable information, carry out health promotion and prevention activities, implement vaccination campaigns, and treat illness—from rural Alaska to urban Bamako. Rigorous research indicates CHWs can do all sorts of complex health tasks, such as delivering birth control injections or HIV care management. And CHWs can ultimately reduce the level of sickness and number of deaths through their efforts.
CHWs are health workers. It’s in the name.
CHWs are an integral cadre of the primary health care workforce, but are often neglected and disconnected from the formal health system—unsupervised, unequipped, and unpaid. So it’s a moral failure too. By 2030, the WHO estimates a global shortfall of 10 million health workers. With salaries, skill, supervision, and supplies, CHWs are poised, ready, and key to help fill that gap. So there’s not a shortage of labor. Instead, there’s an excess of exploitation. The global community seeks to provide health care “on the cheap” at the expense of the CHWs delivering it. The status quo perpetuates a nasty cycle where CHWs are underpaid and consequently devalued.
Financing remains one of the most significant systematic barriers to scaling and sustaining community health services. Africa alone sees a $4 billion financing gap for community health. Worldwide, CHWs face essential medicine stock-outs 1/3 of the time. These widespread shortcomings in community health programs result in CHWs being absent, ill-equipped, or facing grave dangers—like the lack of PPE during COVID.
At Community Health Impact Coalition (CHIC) we’re making professional CHWs (proCHWs)—those that are salaried, skilled, supervised, and supplied—the norm worldwide. We want to see at least 40 low- and middle-income countries adopt proCHW best practices into national policy. Our vision is quality care for all, including those who provide it. We’re calling for decision-makers to join us—the thousands of CHWs and dozens of aligned global health organizations that make up CHIC—on this mission at the 3rd International Community Health Worker Symposium and beyond.
CHIC is supporting content at the Symposium focused on health policy and systems support to advance the proCHW movement. We’re leading a plenary session which will address why the current status quo in community health delivery is broken. By engaging policymakers and CHWs, we will explore specific examples of countries that are bucking the trend and providing the health policy and systems support that CHWs need to deliver quality care for all. We’ll also run a CHW Advocates-centered session, showcasing examples of CHW-led advocacy, organizing, and mobilizing and the impact it’s created. We hope to inspire ministries and partners to include CHWs in decision-making, and to inspire CHWs themselves to champion efforts towards the health policy and systems changes they need and deserve.
Through the sessions we are supporting and our joint advocacy work on the ground we are calling on attendees to:
- #proCHWs - Implement the recommendations of the WHO CHW Guidelines and ensure CHWs are salaried, skilled, supplied, and supervised.
- #CountCHWs - Develop functional and institutionalized National Georeferenced Community Health Worker Master Lists.
- #InvestinCHWs - Expand CHW-focused funding allocations for primary health care delivery, including for community-level supply chains.
- #PayCHWs - Remunerate CHWs fairly for their work - every $1 invested in CHWs returns $10 to the economy.
- #CHWAdvocates - Include CHWs in all decisions that impact them, including policy, planning, and implementation.
- #HealthForAll - Remove user fees and formalize commitments toward universal health care.
Journalist Barbara Ehrenreich once noted that “when someone works for less pay than she can live on— when, for example, she goes hungry so that you can eat more cheaply and conveniently—then she has made a great sacrifice for you, she has made you a gift of some part of her abilities, her health, and her life.” To be a member of the working poor, currently to be a CHW in many countries across the world, is to be an anonymous donor, a nameless benefactor, to everyone else. We’re looking forward to a world in which CHWs are no longer the leading philanthropists, and instead are recognized and valued as the professionals they are. But system change on this scale is a team sport, so meet us at the Symposium and join our team.
