To Eliminate Malaria, We Must Invest in Community Health Workers During COVID-19
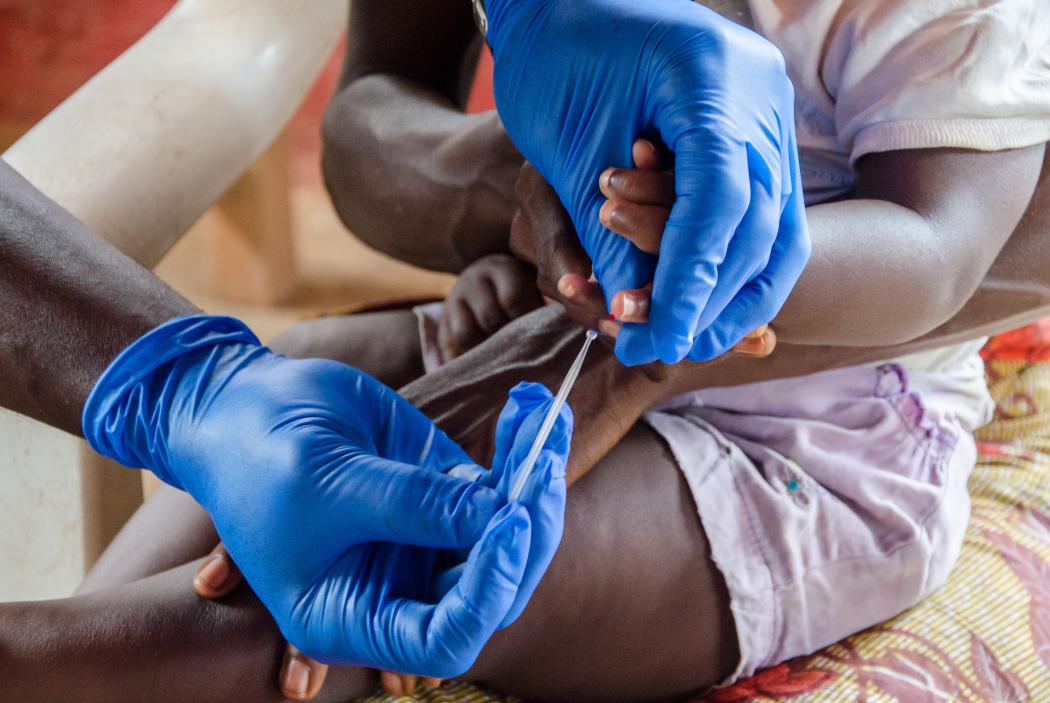
A community health worker conducts a rapid diagnostic test for malaria on a child in Liberia. Photo credit: Last Mile Health.
In countries around the world, the fight against malaria is often waged at the community level, where community health workers (CHWs) diagnose and treat their neighbors to ensure this preventable disease doesn’t become deadly. Their work is part of a global movement to eliminate malaria—which is making slow but steady progress, according to the World Health Organization. However, the growing COVID-19 pandemic, which threatens to overwhelm health systems where malaria is still endemic, could halt this progress.
During the 2014-2016 Ebola outbreak, health systems in Guinea, Liberia, and Sierra Leone were overwhelmed. Tragically, over 28,000 people contracted the virus and over 11,000 people died. Communities were not just devastated by the virus itself, but also by the impact it had on access to health care. The epidemic reduced access to health services, due to the closure of health facilities, fear of seeking care at the facility, and health worker shortages. As access to health care was reduced, it is estimated that malaria-attributable mortality rates increased by 48.0% in Guinea, 53.6% in Liberia, and 50.0% in Sierra Leone. As the COVID-19 pandemic continues, rates of mortality from malaria in low and middle-income countries around the world might even worsen if essential health services are not maintained during the response to the novel coronavirus.
The Ebola outbreak demonstrated the importance of establishing resilient health systems that ensure access to primary health services at the community level via CHWs. Supporting and investing in CHWs—residents of rural communities skilled in the provision of life-saving health services—is vital to maintaining equitable access to care. Their integration into the formal health system expands quality care to the most remote communities, reduces the shortage of health workers, and alleviates the pressure in overwhelmed health centers and hospitals. They were critical to responding to the West African Ebola outbreak, and are now working to detect, prevent, and respond to COVID-19 at the community level.
In Liberia, the deployment of CHWs through the Government of Liberia’s National Community Health Assistant Program—supported with supplies, supervision from clinic-based nurses, and payment—as demonstrated a positive impact on access to quality care. A study evaluating the impact of paid, supplied, and supervised community health workers in Rivercess County, Liberia found that the proportion of children receiving care from a qualified provider increased substantially. In 2018, one out of five malaria cases, reported nationally, in children under-five were diagnosed by CHWs at the community level. This progress must continue during the COVID-19 pandemic.
Health systems must be supported to continue providing essential health services during the current pandemic—otherwise the global progress to eliminate malaria and other preventable diseases will stall, or even reverse. Countries should invest in their community health workers—which includes ensuring they have the personal protective equipment to keep safe, and keep serving their communities—to ensure progress continues.
Community health workers have shown us time and again that they can serve their communities. As we mark World Malaria Day, we must support them to not only fight this current pandemic, but also continue the essential work of ending a preventable disease like malaria.
