Clean Hands Count for Frontline Health Workers
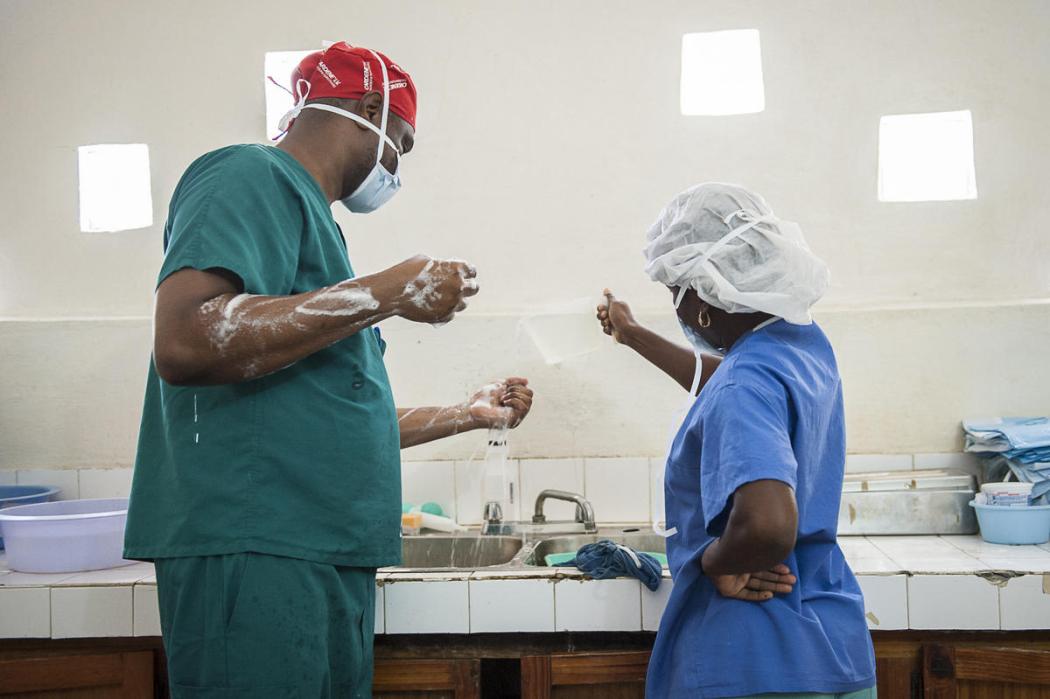
A nurse pours water from a pitcher to help the surgeon scrub for a cesarean section at St. Therese Hospital in Central Plateau, Haiti. © 2014 C. Hanna-Truscott/Midwives for Haiti, Courtesy of Photoshare
The ongoing Ebola response in the Democratic Republic of Congo is again drawing international attention to one of the most important things that health workers can do to keep themselves and others safe—wash their hands. Proper hand hygiene, as defined by the World Health Organization (WHO), can prevent the spread of infections, including health care-associated infections and ones that can lead to outbreaks.
Hand hygiene is a critical component of global health security. However, an estimated 60% of health workers globally are not adhering to correct hand hygiene practices. In many settings, the root causes include a lack of supplies and infrastructure (such as handwashing stations, piped water, and soap or handrub), high patient caseloads, and limited investments in hygiene behavior change. Only six of the 52 countries that reported water, sanitation, and hygiene (WASH) expenditures in the 2017 GLAAS report provided data on expenditures specifically for hygiene, and a 2018 study found that 66% of health facilities in low-and middle-income countries lack soap and piped water for handwashing.
In 2018, the UN Secretary General issued a call to action for WASH in all health facilities. stating, “A recent survey of 100,000 facilities found that more than half lack simple necessities, such as running water and soap —and they are supposed to be health care facilities. The result is more infections, prolonged hospital stays, and sometimes death. We must work to prevent the spread of disease.” This call has been followed by a global response from the WHO, UNICEF, and national governments to improve access to water, sanitation, and hygiene in all health facilities.
At the Global Handwashing Partnership’s Handwashing Behavior Change Think Tank in October, sessions highlighted the need for a realistic, context-based and empathetic approach to behavior change solutions. Robert Dreibelbis of the London School of Hygiene and Tropical Medicine called for handwashing behavior change initiatives to respond to factors that motivate health workers to wash their hands, in contrast to the frequently didactic methods currently in use. Read our 2017 Research Summary for more examples of provider-level behavior change initiatives.
WaterAid Malawi’s Clean Campaign Initiative, which employs participatory behavior change programs and knowledge exchange systems for government and health officials at national and subnational levels to effect hygiene behavior change in health facilities, is one example. At the Think Tank, Allison McIntyre with WaterAid showed how WASH improvements fit into a health systems-wide response. Urgent action for WASH improvements in the health system must include leadership and political will, governance and accreditation, monitoring and targets, research and learning exchange, as well as context-based, affordable technology solutions, such as mobile handwashing stations.
The 2017 global burden of disease study shows that only half of the world’s countries have a sufficient health workforce to provide quality care, but health workers increasingly need to respond to a wide and changing range of public health crises. Read this Lancet editorial for a quick but compelling look at the global health landscape and the range of challenges that health workers are faced with. This shows that we need to be ready to take on new challenges while speeding up progress against long-standing health challenges.
To be prepared for the future, health workers need training, supplies, and support. They also urgently need something we often take for granted—water, sanitation, and hygiene. Access to WASH infrastructure and specific behavior change initiatives must be a core component of any support to health workers, particularly in emergency situations.
Learn more and contribute knowledge on handwashing in health facilities on the Global Handwashing Partnership’s resources hub.
