Advocates of Universal Health Coverage Push for Clear Milestones, Accountability
As policymakers, advocates, and other global health stakeholders have descended on New York and the United Nations this week, two words seem to sum up the conversations around universal health coverage (UHC):
“Now what?”
From the years of clamoring for UHC to be a central priority in global health policy to the breakthrough 2012 UN resolution urging countries to prioritize UHC, Sustainable Development Goals target 3.8 in 2015, the Astana Declaration last year, and the adoption of the Political Declaration for the High-Level Meeting on UHC this week, we’ve seen a step-wise approach to taking UHC from words on paper to real commitments, policies, and investments to make it a reality.
With the new commitment made on Monday at the UN, and how it will be done still pretty fuzzy, the “Now what?” question takes on outsize importance.
We believe health workers are at the heart of health for all.
How much these global commitments to UHC really drive change toward universal access to high-quality, essential health services and the affordability of those services depends on how well we collectively answer the question. While the political declaration does mention the need to address many of the components necessary to achieving UHC, the direct policy and financial commitments needed to meaningfully address those components are lacking.
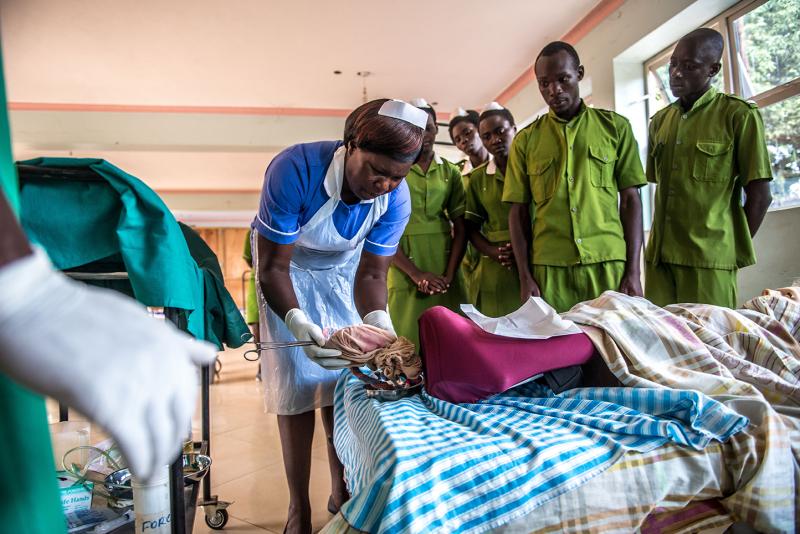
Midwife Beatrice Aciro conducts a practical exercise with students at the Good Samaritan School of Nursing & Midwifery in Uganda. Photo by Tommy Trenchard for IntraHealth International.
To us, this is in part because of the complexity of issues under the UHC umbrella—from health workforce education and training to supply chain, service cost, service demand and uptake, and safety and labor issues. All of these components require separate, clear milestones, targets, and data that are brought back together under the UHC umbrella so advocates can collectively drive policymakers to achieve them and hold policymakers accountable if they do not.
IntraHealth International, as well as the advocacy coalitions we manage secretariats for—the Frontline Health Workers Coalition and Safeguarding Health in Conflict Coalition—focuses our work on what we believe is the heart of health for all: health workers on the front lines of communities that are furthest from UHC.
Ahead of the Global Conference on Primary Health Care in Astana last October, the Frontline Health Workers Coalition identified four actions that are central to achieving sustainable access to the frontline health workforce teams needed to deliver high-quality health services to all.
We also know the ability of health workers to deliver those services depends on whether they are safe to perform their jobs, and the Safeguarding Health and Conflict Coalition has documented a worrisome and perhaps worsening trend of attacks on health workers in countries that are in conflict.

Outside a village health center in Uttarakhand, India, auxiliary nurse midwife Saraswati Rawat (left) gives a measles rubella vaccine to a young boy. Photo by Vijay Kutty for IntraHealth International.
Case in point: in 2018 we called for far greater action to protect health workers in the Democratic Republic of the Congo, as militants were deliberately targeting Ebola workers and interfering with the Ebola response. Since then, there have been more attacks and at least 2,000 people have died from the virus. Member States and the UN Security Council must take immediate action to halt attacks on health care, which occurred in at least 23 countries in 2018, for UHC to be possible.
Similar breakdowns of the crucial components of other key issues for UHC, such as gender-related barriers to accessing care, have also been recommended by advocates. Commitments across the components of UHC need to be collected, agreed to, and pushed collectively by health and development advocates around the world.
More importantly, recommendations to address the core components of UHC globally need to be teased out further at the country and regional levels to estimate as accurately as possible the investments and policy changes required. Where data is inadequate to push such recommendations, we need to advocate for rapid provision of such data.

Health workers provide family planning counseling and services at CSPS Dassasgho in Ouagadougou, Burkina Faso. Photo by Trevor Snapp for IntraHealth International.
To accomplish this, civil society—especially in communities furthest from achieving UHC—needs to be far better supported by governments, donors, and fellow advocates to accurately portray local needs.
“Now what?”
Now comes the hard work. Advocates must go back home and push for data, milestones, and targets.
IntraHealth staff, our partners, and members of the coalitions we help lead have seen firsthand the devastating consequences that occur when the complexity of an issue like the health workforce leads to inaction by policymakers.
We cannot allow this to happen in the UHC movement.
This post was originally published on Medium by the UHC Coalition.
This piece is also part of IntraHealth's celebration of 40 years of commitment to health workers. Follow along: #TheFutureOf #IntraHealth40 #HealthWorkersCount
